The Big Three Menopause Triggers Testing and Video Training
$1,175.00 Original price was: $1,175.00.$1,075.00Current price is: $1,075.00.
The three most common triggers for hormone imbalance includes food sensitivity, gut pathogens and toxicity. With the bundle, you’ll get all three test kits and three comprehensive video recordings, showing you how to read and interpret your test results. You will also get personalized recommendations emailed to you directly with your suggested protocol for each individual test.
Learn More Below…
Gluten-Associated Cross-Reactive Foods and Food Sensitivity
Gluten can easily be considered the mother of all food sensitivities but what many are not aware of is the cross reactive sensitivities that can be wreaking the same havoc on your body functionally. Gluten associated cross reactive sensitivities develop based on the immune system dysregulation created by a long term consumption of gluten when one is gluten sensitive. This immune system dysregulation can position your body to create an autoimmune reaction to molecules that are similar to gluten, thus causing the same function health issues, such as:
- Malabsorption
- Leaky gut
- Autoimmunity
- Adrenal insufficiency
- Chronic inflammation
- Brain degeneration
- and so much more…
Here at Depke Wellness we routinely test gluten associated cross reactive sensitivity and recognize that over 95% of your clients tested have unknown food sensitivities. I also want to note why this is essential to test. What most do not know is that approximately 86% of the people struggling with food sensitivity are actually asymptomatic. So basically, so many people are making food choices that are leading to chronic illness with little to no recognition. It’s time you find this out.
Here is the list of potential gluten associated cross reactive foods:
|
|
|
Specimen Requirement: Collect: 5 mL red top or tiger top |
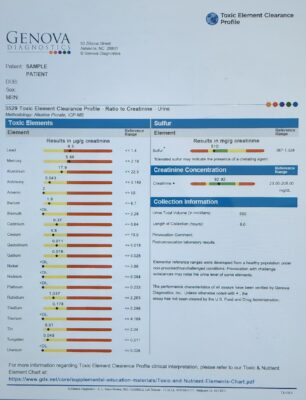
Toxic Element Clearance Profile #3529
Sample Report Below:
GI Effects™ Microbial Ecology Profile w/H.Pylori Add On – Stool
A Targeted Stool Test for Optimal Clinical Utility
The GI Effects Microbial Ecology Profile is the most comprehensive stool test that assesses the diverse gut microbiome. Results provide immediate, actionable clinical information for the management of detectable parasites, bacteria, and yeast, as well as providing valuable assessment of gut microbiota via 24 Commensal Bacteria targets.
The GI Effects Microbial Ecology Profile is part of the larger GI Effects Comprehensive Stool Profile, which also provides information about digestion, inflammation, and bacterial metabolism markers. A larger fecal biomarker panel such as the GI Effects Comprehensive Stool Profile offers the advantage of assessing multiple functional areas that may be contributing to symptoms. For example, diarrhea could stem from multiple causes including pancreatic exocrine insufficiency, inflammation, food allergies, or the presence of a pathogenic or potentially pathogenic organism.
Genova Diagnostics is excited to announce the addition of polymerase chain reaction (PCR) for parasites to the GI Effects Profiles. PCR is a highly sensitive and specific methodology that detects an organism’s DNA.
The GI Effects now includes 6 PCR targets that detect common protozoan parasites:
- Blastocystis spp. with reflex subtyping 1-9
- Cryptosporidium spp.
- Cyclospora cayetanensis
- Dientamoeba fragilis
- Entamoeba histolytica
- Giardia
The 6 PCR targets replace the 3 EIA biomarkers. The GI Effects upgrade also includes several report enhancements for ease of use.
Why Choose Genova Diagnostics’ Gastrointestinal Products?
- GI Effects is a comprehensive assessment of complete GI health, assessing the root cause of most gut complaints.
- Genova uses a combination of PCR, culture, and microscopic methods to ensure any and all relevant organisms are identified.
- Genova recovers live organisms (yeast and bacteria) for susceptibility testing and improved treatment options.
- Genova measures metabolomics and can assess the interaction between the microbiome and its host.
- Genova is the market authority on stool inflammatory markers, testing calprotectin, EPX and sIgA.
- Genova has amassed a database of hundreds of thousands of complete stool profiles. Our data driven and evidence-based analysis ensures the highest standard of analytical validity and clinical utility.
When Should the GI Effects Microbial Ecology Profile Be Considered?
Patients with a clinical history suggestive of a gastrointestinal infection or dysbiosis can be evaluated with the GI Effects Microbial Ecology Profile. Symptoms such as gas, bloating, abdominal pain, diarrhea, and constipation may be a result of a microbial imbalance or infection. This profile can also be used to monitor treatment efficacy to eradicate an organism or to monitor changes to the microbiota.
Gut microbes are codependent with one another and with their human host, and the health of one affects the other. A sizeable volume of research associates a dysbiotic, or imbalanced gut microbiome with multiple disease states both within and outside of the GI tract.1,2 The microbiome’s diverse metabolic activities ultimately impact the human host, and the human hosts activities ultimately affect the microbiome’s health.
The GI Effects Microbial Ecology Profile biomarkers include:
- Commensal Bacteria demonstrate the gut microbiomes composition and relative abundance.
- More than 95% of commensal gut organisms are anaerobic and are difficult to recover by traditional (aerobic) culture techniques. Polymerase Chain Reaction (PCR) methodology identifies bacterial populations and is considered the standard for anaerobic bacteria assessment.
- GI Effects assesses a set of 24 genera/species that map to 7 major phyla.
- Bacterial and mycology cultures demonstrate the presence of specific beneficial and pathological organisms.
- Bacterial and mycology sensitivities are provided for pathogenic or potentially pathogenic cultured organisms. The report includes effective prescriptive and natural agents.
- Parasitology includes comprehensive testing for all parasites on every parasitology exam ordered.
- GI Effects provides microscopic fecal specimen examination for ova and parasites (O&P), the gold standard of diagnosis for many parasites.
- 6 Polymerase chain reaction (PCR) targets detect common protozoan parasites including Blastocystis spp. with reflex subtyping 1-9, Cryptosporidium spp., Cyclospora cayetanensis, Dientamoeba fragilis, Entamoeba histolytica, and Giardia. PCR for organisms is emerging as a highly sensitive method for infectious organism detection.
- Selection of a one-day or three-day sample collection is based on the clinician’s clinical index of suspicion for parasitic infection. If there is no/low suspicion, a one-day sample will likely be adequate. For high suspicion, a three-day sample collection is optimal.
- Additional Biomarkers Available:
- Campylobacter
- Clostridium difficile
- Escherichia coli
- Helicobacter pylori
- Macro Exam for Worms
- KOH Preparation for Yeast
- Zonulin Family Peptide
- Fecal Lactoferrin
What Advantage Does the Microbial Ecology Profile Offer Compared to Other Diagnostics?
GI Effects® represents the best technical available to assess the gut microbiome, combining:
- 16S rRNA gene polymerase chain reaction (PCR) amplification technique for anaerobic commensal bacteria
- Matrix Assisted Laser Desorption Ionization Time-of-Flight Mass Spectrometry (MALDI-TOF MS) technology for bacterial and fungal species identification via culture
- Gold standard microscopic ova and parasite (O&P) detection
- Real-time PCR for the identification of 6 common parasites
- Next-Generation DNA sequencing for Blastocystis spp. with reflex subtyping 1-9
The test report is organized so that the clinician can move through results in a logical order that enhances clinical utility, starting with the innovative Interpretation-At-A-Glance pages to synthesize the information.
What Can Clinicians and Patients Expect from GI Effects Microbial Ecology Profile Stool Testing?
The GI Effects Microbial Ecology Profile results provide insight into the root cause(s) of gut symptoms originating from a disturbed gut microbiome. Symptoms often improve as identified imbalances become normalized through targeted antimicrobial, dietary, lifestyle, and supplementation therapeutics.
References
- Marchesi J, et. al. The gut microbiota and host health: a new clinical frontier. Gut. 2016 Feb;65(2):330-9.
- Clemente J, et. al. The impact of the gut microbiota on human health: an integrative review. Cell. 2012 Mar;148(6):1258-70.
H.Pylori Add On
Non-invasive Assay
Stool antigen tests have been recommended by both the American Gastroenterological Association (AGA) and the American College of Gastroenterologists (ACG) as the most accurate non-invasive tests for diagnosis and for confirmation of eradication.1,2 This method is highly sensitive and specific and useful for diagnosis, therapeutic monitoring, and test of eradication.
Unlike stool antigen tests, Serology-based methods have a sensitivity and specificity of only 90% and cannot distinguish between active and resolved infection.3,4 Thus, serology tests are not recommended by the AGA for initial diagnosis of H pylori infection.4 Furthermore, they are not recommended by either the AGA or the ACG for monitoring infection or confirming eradication of the organism.3,4
Transmission
Is incompletely characterized. Person-to-person transmission is most commonly implicated with fecal/oral, oral/oral, or gastric/oral pathways.
Symptoms
Acute gastritis with abdominal pain, nausea, and vomiting. Non-ulcer dyspepsia is common. Development of severe H. pylori disease is partially determined by the virulence of the infecting strain.
Therapeutic Considerations
Conventional recommendation is polypharmacy: antibiotics and proton-pump inhibitors (PPIs). See www.acg.gi.org.
Botanical anti-H. pylori formulas may prove helpful. See www.cdc.gov/ulcer/keytocure.htm.
Test Type: StoolTest
1)Talley NJ; American Gastroenterological Association. American Gastroenterological Association medical position statement: evaluation of dyspepsia. Gastroenterology. 2005;129:1753-1755.
2) Chey WD, Wong BC; Practice Parameters Committee of the American College of Gastroenterology. American College of Gastroenterology guideline on the management of Helicobacter pylori infection. Am J Gastroenterol. 2007;102:1808-1825.
3)Talley NJ, Vakil N; Practice Parameters Committee of the American College of Gastroenterology. Guidelines for the management of dyspepsia. Am J Gastroenterol. 2005;100:2324-2337.
4)Talley NJ, Vakil NB, Moayyedi P. American Gastroenterological Association technical review on the evaluation of dyspepsia. Gastroenterology. 2005;129:1756-1780.
Be the first to review “The Big Three Menopause Triggers Testing and Video Training” Cancel reply
Related products
Test Kits








Reviews
There are no reviews yet.